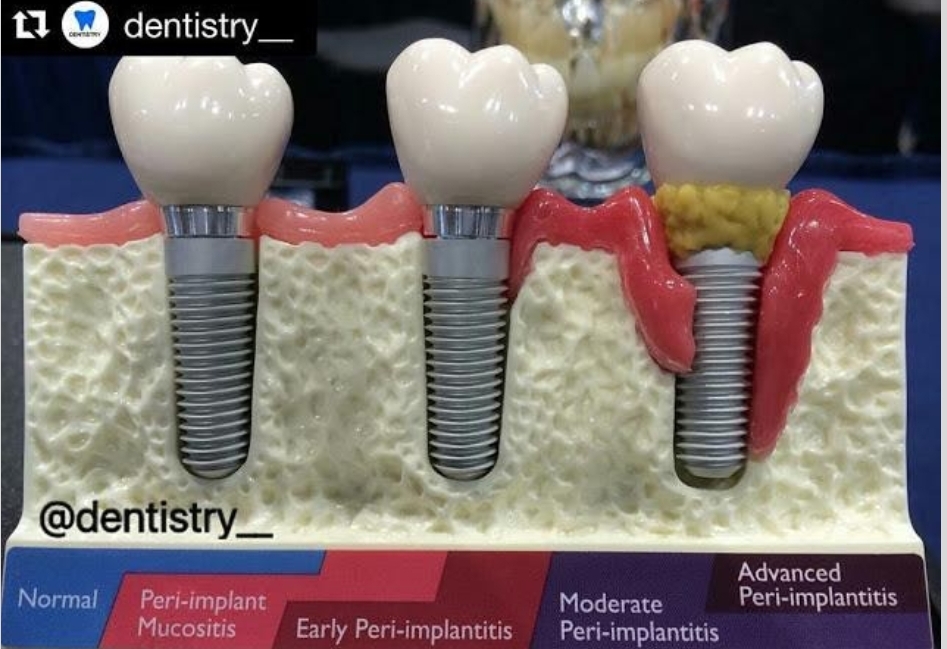
Dental implants are fantastic, but like anything biologic or placed in or on the human body can NOT always be completely predictable or guaranteed all the time. One of the long-term risks associated with dental implants is a condition called Peri-implantitis.
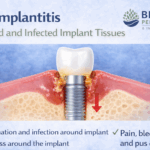
Peri-implantitis is an infectious disease that causes inflammation of the surrounding gum and bone of a dental implant, and can lead to the loss of supporting bone. This condition is very difficult to treat.
Fortunately, most patients receiving dental implants never develop this condition. Sometimes, for a variety of reasons, bone can be lost around a dental implant. This will often occur without a patient ever being aware of it. Some dental implants will develop bone loss very early after having the implant crown is placed or it can happen many years down the road. Most patients are unaware that they have bone loss around the dental implant. Peri-implantitis generally begins painlessly and without symptoms. Once peri-implantitis becomes advanced, symptoms can develop and the patient will notice.
There are several risk factors for peri-implantitis, especially smoking. Smoking definitely causes constriction of blood vessels which leads to bone loss. Medical issues such as Diabetes, Osteoporosis and a weakened immune system are more at risk for developing bone loss around dental implants. Those with a history of gum disease are more at risk.
Good home care is critical. Brushing twice a day for 2 minutes or more with an electric toothbrush, flossing once a day and using adjuncts such as a rubber tip or implant floss every day! Grinding your teeth is another risk factor for dental implant bone loss. Factors related to the surgical procedure can also cause peri-implantitis to later occur: Soft bone, lack of tightness when the dental implant is placed, bone that was grafted in a vertical fashion, implant size too big, overheated bone, and many others.
Signs of Peri-implantitis
• Deep periodontal pockets around the implant
• Pus comes out from the implants and gums
• Bleeding at the gumline
• Appearance – Gum tissue may appear red, or slightly purplish bluish, and tartar/plaque build up is noted
• Progressive loss of supporting bone on x-rays
• Metal thread exposure
• Long tooth
Again, peri-implantitis is not always symptomatic and typically there is no pain. Some patients will complain of a dull ache or tenderness when they brush or touch the area. A bad taste can develop if infection or pus has developed around the implant. If this infection around the implant becomes very severe, the glands in your neck may become swollen and the dental implants may begin to be noticeably loose.
The first thing an implant specialist will usually check around the implant is to make sure the crown or bridge was made properly. An x-ray, or sometimes a 3-D Cone Beam CT scan is necessary to see the inside surface. Extra cement can often be the cause of peri-implantitis. The cement oozes beyond the abutment and gets down below the gum near the bone and becomes an irritant. There is often good reason to make crowns held in by screws rather than cement in some cases. The technique of cementation and choice of cement used is a big factor on implant success!
This is why it is important to work with an experience implant specialist and restorative dentist in implant placement.
Occasionally a loose abutment screw may be present which may not have been torqued properly or it has broken, sometimes due to a patient’s heavy bite. Patients with heavy bites need to have their crowns designed to protect the implants.
How an implant crown is made is critical for the longevity of the dental implant in the bone. Low-budget implants have poorly designed screws or may move (even microscopically) when you chew.
Sometimes gum disease on nearby teeth can stimulate peri-implantitis to start on the implant. Generally some type of exploratory surgery needs to be done to find out the cause of peri-implantitis along with a simultaneous bone graft to save the implant. Not all implants that have developed peri-implantitis can be saved.
Treatment
The long-term goals are to stop the progression of bone loss and maintain your dental implants! Generally speaking the area will need to be cleaned thoroughly using dental instruments. Sometimes antibiotics will be prescribed or special antibacterial agents will need to be applied to the implants itself such as iodine or tetracycline.
Sometimes a laser procedure can be performed around the implant, called LAPIP, to sterilize the implant. Most peri-implantitis dental implants require surgery and bone grafting. This means that the dental implant surgeon has to open the gum tissue in order to detoxify the implant. All of the bacteria will be killed in order to have bone re-grafted onto the implants. The physiology and the type of bone that is used is critical. Sometimes your implant surgeon will recommend using your body’s own helpful blood products such as PRF/ PRP. The best way to prevent peri-impantitis is to have the implant properly placed by a specialist and restored by a highly experienced restorative dentist. Oral surgeons and periodontists have extensive training and have also developed more predictable implant placement technique. When an implant has had too much bone loss, a success rate can be as low as 35 to 50%. Some severe cases of peri-implantitis are better off removing the implant and placing a new one if detoxifying and regrafting do not seem to have a good long-term prognosis. If one implant fails or develops bone loss, it doesn’t mean the second one will. Time will tell if the procedure works. There are no guarantees on grafting around implants that have pre-existing bone loss. It is far more successful if the bone missing is in the shape of a moat rather than an entire wall missing.
Correction of dental implants with problems should be performed by an implant specialist and highly trained restorative dentist who routinely performs this procedure. Dr. Todd Britten is a periodontist and implant specialist practicing in Clearwater, Florida. As periodontist, Dr. Britten specializes in the prevention, diagnosis, and treatment of periodontal disease, the placement of dental implants and bone grafts, and treatment of oral inflammation. Periodontists also perform cosmetic periodontal surgery. Dr. Britten has received an additional three years of specialty education and surgical training beyond dental school and has experience in treating this very difficult condition. If you have any questions regarding implant placement, contact us at 727-586-2681 or email us at .