Dr. Todd Britten Hosting 10th Annual Veterans Day Event In recognition of Veterans Day, Clearwater periodontist and dental implant specialist Dr. Todd Britten will offer complimentary periodontal screenings, consultation and treatment to local veterans. The goal of this annual event...
🦷 Protect Your Dental Implants: Understanding Peri-Implantitis🦷 Peri-implantitis is a condition that affects the tissues around dental implants, leading to inflammation and bone loss. If left untreated, it can jeopardize the stability of the implant. Signs to Watch For:...
🔍Understanding Periodontal Abscesses 🔍 Do you have persistent pain in your gums? It might be more than just a toothache! A periodontal abscess is a localized infection within the gums, often causing swelling, pain, and discomfort. 🤕 Signs to...
What is Guided Bone Regeneration? Guided Bone Regeneration (GBR) is a dental procedure used to help rebuild bone in areas where it is lacking, often to support a dental implant. Here's a simplified explanation: 1. Purpose: Sometimes, a...
COCOFLOSS: Buy from Cocofloss.com CVS Store locator: Cocofloss Store Locator Amazon Store: Cocofloss LISTERINE ULTRACLEAN FLOSS: Tight spaces/Good for those spaces that other floss shreds easily. Usually available at Target, CVS, Publix, Walmart and Walgreens. Order online at Amazon here: Amazon...
Interdental Aids: What's Your Type? When selecting the size for an interdental aid, such as a Soft-Pick or interdental brush, aka proxabrush, consider the width of the spaces between your teeth. It's often a good idea to start with a...
The Oral Hygiene Olympics: Gold Medalists! Welcome to the Oral Hygiene Olympics, where we honor the unsung heroes that keep our smiles bright and healthy! After fierce competition, we're excited to announce the gold medalists in each category: Best Toothpaste:...
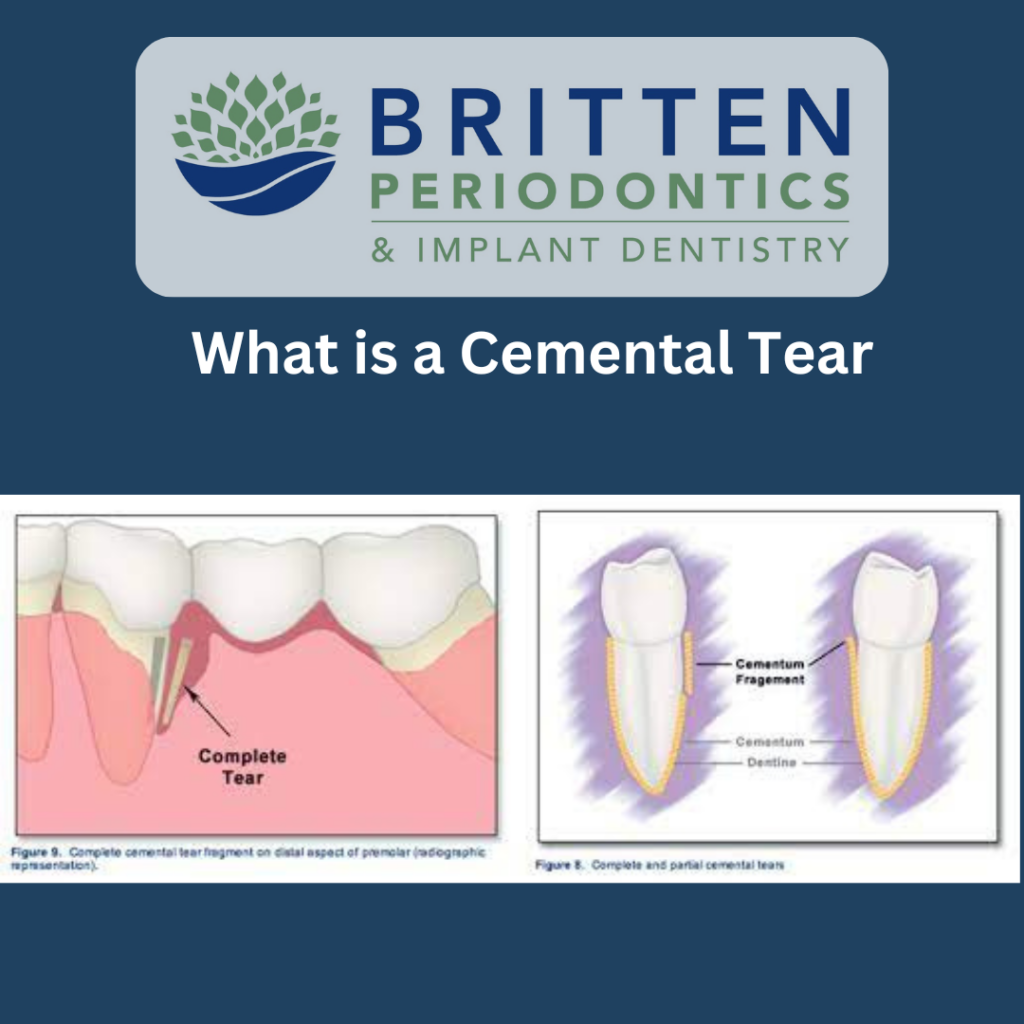
Understanding Cemental Tears: Protect Your Oral Health Have you ever heard of a cemental tear? It's a rare dental condition that can have serious consequences for your teeth. Here’s what you need to know: What is a Cemental Tear? A...
Back to School Drive *NEW* Make a donation to A Kid's Place directly through Amazon here: https://www.amazon.com/hz/wishlist/ls/3Q4EQ1M2VMTG5?ref_=wl_share WHAT: In partnership with A Kid’s Place Tampa Bay, we are collecting back-to-school items WHEN: Collection Dates July 1st –...
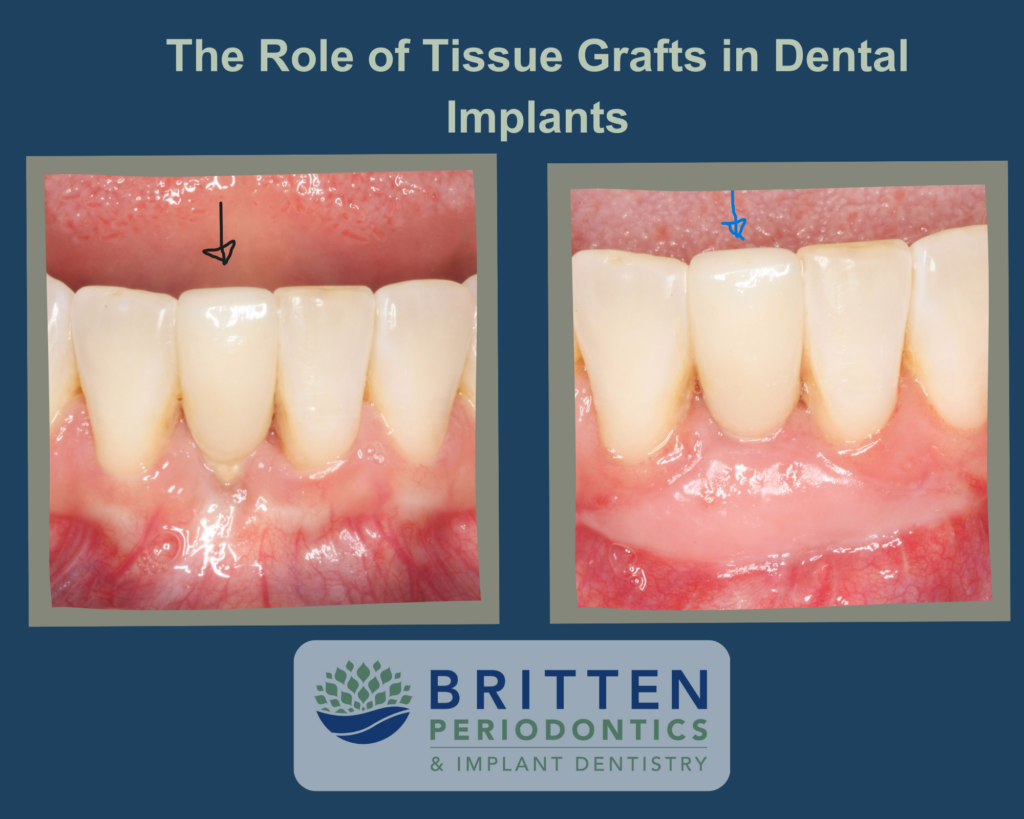
Enhancing Dental Implant Success: The Role of Tissue Grafts in Dental Implants A free gingival graft on a dental implant is aimed at improving the amount of attached gingiva (gum tissue) around a dental implant. This can be necessary for...