Medications & Dry Mouth: The Hidden Threat to Your Oral Health
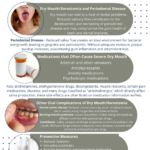
Medications used to treat conditions such as ADHD, depression, anxiety, and other psychiatric disorders can have a significant impact on oral health. One of the most common side effects of these drugs is xerostomia, or dry mouth, which can lead to a host of dental problems. The reduced saliva flow caused by these medications contributes to the development and worsening of periodontal disease, dental caries, burning mouth syndrome, and candidiasis. Understanding the risks and taking preventive measures is crucial for maintaining oral health while undergoing treatment with these medications.
Medications That Cause Dry Mouth
Several classes of medications are known to reduce saliva production, including:
- – Adderall and Other Stimulants – Used for ADHD, these drugs increase dopamine and norepinephrine levels but also lead to dehydration and dry mouth.
- – Antidepressants – Selective serotonin reuptake inhibitors (SSRIs), tricyclic antidepressants, and monoamine oxidase inhibitors (MAOIs) are known to decrease saliva production.
- – Anxiety Medications – Benzodiazepines and other anxiolytics have a drying effect on the oral mucosa.
- – Psychotropic Drugs – Medications used for schizophrenia and bipolar disorder, such as antipsychotics and mood stabilizers, can significantly reduce salivary flow.
Oral Health Complications
- Periodontal Disease
- Saliva plays a crucial role in maintaining the health of the gums by neutralizing acids and providing antibacterial protection. Reduced saliva flow creates an ideal environment for bacterial overgrowth, leading to gingivitis and periodontitis. Without adequate moisture, plaque buildup increases, exacerbating gum inflammation and attachment loss.
- Dental Caries
- Dry mouth promotes tooth decay by reducing the natural cleansing action of saliva. The lack of saliva allows bacteria to thrive, increasing the risk of cavities, especially along the gumline and between teeth. Patients taking dry mouth-inducing medications should be vigilant about fluoride use and regular dental checkups to prevent decay.
- Burning Mouth Syndrome
- A persistent burning sensation in the mouth is another side effect of dry mouth. This condition is often seen in patients taking psychotropic medications, and the discomfort can be exacerbated by a lack of saliva. Burning mouth syndrome can significantly impact a patient’s quality of life, making eating and speaking difficult.
- Candidiasis (Oral Thrush)
- Saliva contains antifungal properties that help control Candida growth in the mouth. When saliva production is compromised, fungal infections become more common, leading to white patches, soreness, and discomfort. This condition is particularly problematic for individuals on long-term psychotropic or stimulant medications.
Preventive Measures
- To mitigate the oral health risks associated with dry mouth medications, consider the following strategies:
- – Increase Hydration – Drinking plenty of water throughout the day can help maintain oral moisture.
- – Use Saliva Substitutes – Artificial saliva products or sugar-free gum with xylitol can stimulate saliva production.
- – Maintain Excellent Oral Hygiene – Brushing twice daily with fluoride toothpaste and flossing regularly can help reduce bacterial buildup.
- – Regular Dental Checkups – Seeing a dentist regularly for professional cleanings and fluoride treatments can help prevent complications.
- – Avoid Alcohol and Caffeine – These substances can exacerbate dry mouth and should be consumed in moderation.
- – Strongly consider weaning off any offending medications if possible (consult with physician)
Conclusion
Medications used for ADHD, depression, anxiety, and other psychiatric disorders can significantly impact oral health due to their drying effects. By understanding the risks and implementing preventive strategies, patients can minimize the negative effects on their teeth and gums. Consulting with both dental and medical professionals is essential for managing these side effects while continuing necessary medications.