Clearwater Periodontist Expands Services with Advanced Tissue Grafting Techniques
Dr. Todd Britten provides advanced tissue grafting techniques in his Clearwater, Florida practice. Patients will benefit from these innovative procedures designed to restore gum health, enhance oral function, and improve esthetic concerns.
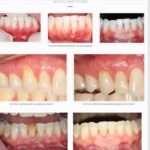
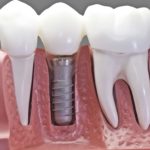
Tissue grafting is a critical procedure for addressing gum recession, restoring lost tissue, and improving the stability of teeth. These highly specialized techniques include connective tissue grafts, free gingival grafting and even grafting around dental implants. He uses the latest advancements in periodontal science to offer superior results with minimal discomfort.
“Our goal is to provide our patients with the most effective and comfortable treatments available,” said Dr. Todd Britten, owner at Britten Periodontics and Implant Dentistry. “By incorporating these advanced tissue grafting techniques, we can better address complex cases of gum recession and ensure a high standard of care.”
Key Benefits of Advanced Tissue Grafting Techniques Include:
– Enhanced Precision
– Improved Aesthetic Results
– Faster Recovery
– Increased Success Rates
Dr. Britten encourages patients experiencing gum recession or other periodontal issues to schedule a consultation to learn more about how our new tissue grafting techniques can help. For more information or to book an appointment, please contact us at 727-586-2681.
Britten Periodontics & Implant Dentistry is a leading periodontal practice in Clearwater, Florida, committed to providing exceptional dental care through innovative treatments and personalized attention. Our expert team is dedicated to improving oral health and enhancing the quality of life for their patients.









 https://brittenperio.com/wp-content/uploads/2024/05/2-1.pnghttps://brittenperio.com/wp-content/uploads/2024/05/2-1.png
https://brittenperio.com/wp-content/uploads/2024/05/2-1.pnghttps://brittenperio.com/wp-content/uploads/2024/05/2-1.png

