“Here in our Clearwater periodontal office, we have noticed that many young people and other patients feel that compared to traditional tobacco use, e-cigarettes are a safer and healthier option,” says Clearwater periodontist Dr. Todd Britten. “I see that companies selling these products are adding attractive and sweet flavoring products to attract young people. However, we are noticing in our dental practice that vaping may be as dangerous to oral health—if not more dangerous for the teeth and gums!”
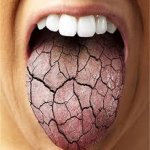
Dr. Britten explained that E-cigarettes and vaporizers work by heating a liquid to generate aerosol, rather than smoke. The E-liquid in vaporizers and e-cigarettes are usually made up of propylene glycol, glycerin, flavorings, water, and in e-cigarettes, nicotine. One of the major ingredients used in vapes and e-cigarettes is a fluid called propylene glycol. “It is a like a thin sweet-tasting gel,” says Dr. Britten, “which when broken down becomes acetic acid, lactic acid, and propionaldehyde. We know in the dental community that acids are NEVER good for tooth enamel – that is what causes cavities!” Dr. Britten also explained that it is believed that the water molecules in saliva and the tissues of the mouth will bond to the propylene glycol drying the mouth and its tissues out considerable. “We know well in the dental community how harmful dry mouth is in the development of both cavities and gum disease!”
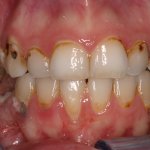
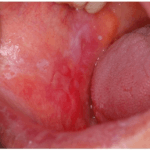
Another ingredient in e-liquid is a combination of vegetable glycerin as well as flavorings which studies have shown produces twice as much plaque on the teeth, which is also known as biofilm, and increased the stickiness of the bacteria to the teeth by about four times! This, he explained, means more cavity-causing bacteria to stick to the teeth and roots and can lead to severe tooth decay as well as an increase of gum disease.
“Even for those who may be quitting smoking by switching to e-cigarettes or vapes, unfortunately, it is not a safer alternative for the teeth and soft tissues inside the mouth,” Dr. Britten says. “Nicotine users using an e-cigarette may have lower concentrations of nicotine in their blood, but we really haven’t seen what vaping and e-cigarettes do to the body long-term.” But short-term, he says, dentists and dental hygienists are starting to see softer enamel, increased plaque and drier mouths with patients using these products. Which is not good for patients, because as Dr. Britten says, the plaque bacteria in the mouth cause gum disease and the combination of these bacteria and acid in the mouth, cause dental cavities.
Britten Periodontics & Implant Dentistry is a periodontal practice offering patients personalized dental care in implant dentistry in Clearwater, Florida. Dr. Todd Britten offers sedation dentistry, which can be very helpful for those needing advanced treatment, suffer from PTSD or have a fear of the dentist.
Questions? Contact us at:
[iphorm id=”3″ name=”Contact form”]