Peri-Implantitis Symptoms You Should Never Ignore
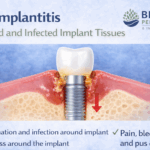
A peri-implantitis symptom often appears quietly, which is why many patients don’t realize there’s a problem until damage has already begun. Peri-implantitis is an inflammatory condition that affects the gum tissue and bone around a dental implant, and early detection makes a major difference.
Common Peri-Implantitis Symptoms
One of the earliest warning signs is bleeding when brushing or flossing around an implant. In addition, the gums may appear red, swollen, or tender. A persistent bad taste or drainage around the implant can also indicate infection. These changes should never be ignored, even if pain is mild or absent.
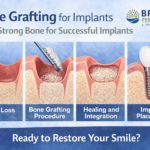
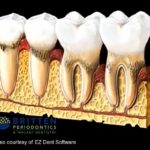
Bone Loss Around the Implant
As the condition progresses, inflammation can lead to bone loss around the implant. This weakens the implant’s support and may cause it to feel loose. At this stage, a peri-implantitis symptom may include discomfort while chewing or changes in how the implant feels when biting down.
Why Peri-Implantitis Develops
Plaque buildup around implants plays a major role. However, a history of gum disease, smoking, diabetes, and irregular maintenance visits can increase risk. Because implants lack the same attachment fibers as natural teeth, infection can spread faster once it starts.
Why Early Treatment Matters
Without treatment, peri-implantitis can lead to implant failure and the need for removal. Early intervention may include deep cleaning, antimicrobial therapy, or laser treatment, depending on severity. Regular periodontal maintenance visits help reduce risk by catching changes early.
If you notice any bleeding, swelling, or changes around an implant, schedule an evaluation promptly. Addressing symptoms early helps protect your investment and your oral health long-term.